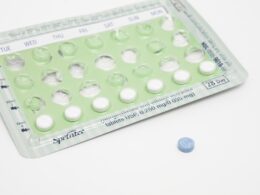
Women choose birth control methods for lots of reasons. Some people prefer nonhormonal options like condoms, diaphragms or cervical caps, while others want a more permanent method like an IUD or vaginal ring.
However, if you’re someone who has an increased risk of blood clots because of age or family history, using hormonal birth control could increase your odds. That includes combined estrogen and progestin pills, the contraceptive patch and the NuvaRing.
1. Pills
Blood clots can be deadly, especially if they break loose and travel to the lungs. This is called pulmonary embolism, and it’s one of the main reasons why women who use the pill — or any hormonal birth control method, for that matter — should be very careful.
The hormones in birth control pills can increase a person’s risk of blood clots by making the blood thicker. But the overall risk of blood clots is still lower than the risk of pregnancy. Combined oral contraceptives (the pill) that contain both estrogen and synthetic progestin, such as drospirenone or desogestrel, are the most likely to cause blood clots. These include brands like Yasmin, Beyaz, and Safyral.
The first 6 to 12 months of hormonal birth control use are when you’re at highest risk of a blood clot. But the risk goes back to baseline after that. People who have a family history of blood clots or conditions that up their risk — like high blood pressure or migraine with aura, for example — should talk to a doctor before using any type of hormonal birth control.
2. IUDs
Blood clots form when proteins in your body act to create a makeshift plug (a thrombus) over an injury or hole. If a clot in the vessels moving blood up from your legs breaks off and travels to your lungs, it’s called deep vein thrombosis or pulmonary embolism (PE). PE can be deadly because it stops blood from getting to your lungs.
Hormonal birth control increases your risk of a blood clot because it contains estrogen, which changes your uterus’s normal clotting mechanisms. But modern combination birth control pills, patches, and rings have lower doses of estrogen than they did a few decades ago.
IUDs are tiny devices made of copper or hormonal materials that slip into your uterus. Most doctors insert them during an office visit. Your doctor may give you pain medication or numb the area before doing so. You can have an IUD inserted at any time during your menstrual cycle, but some women find it more comfortable to get it done while they’re on their period.
3. Implants
Blood clots occur when blood sticks together to form a thick clump that restricts normal circulation. They can be small and stay put, or they could break off and travel to the lungs, blocking blood flow there (a life-threatening condition called pulmonary embolism). Blood clots are often caused by hormones that occur during pregnancy or while taking hormonal birth control.
Doctors aren’t sure why this is, but they think the estrogen in some types of birth control — specifically the combination pill, patch or vaginal ring that has both estrogen and progestin — increases the chances of blood clots by changing how your liver makes clotting factors. This raises your risk about two to six times more than if you don’t use birth control at all.
Some forms of birth control, such as the IUDs made of levonorgestrel or copper and progestin-only methods like the implant, don’t increase your chance of a blood clot. If you have a history of blood clots, your doctor may recommend using one of these methods instead of the combined pills.
4. Vaginal rings
A vaginal ring is a hormone-based birth control that contains estrogen and etonogestrel (a form of progestin different from what’s in low-dose combined oral contraceptives). The ring increases your risk for blood clots by a small amount but so do many other types of hormonal birth control.
The ring is inserted like a tampon and most women can’t feel it. You take it out for a week at the end of your menstrual cycle then insert it again. The ring protects you from pregnancy 96%-99% of the time when you use it correctly and consistently.
It does increase your risk for a clot in the deep vein of your leg (DVT) by a little but it doesn’t raise the risk as much as the pill or patch. A clot in this type of blood vessel is called a pulmonary embolism and is a very serious medical emergency. If you have a history of DVT or a family history of it, talk to your doctor before using a ring, patch or pills. They can tell you what other forms of birth control might be safer for you.
5. Other methods
The good news is that even though blood clots are very dangerous, they’re also very rare. It’s important to understand what causes a blood clot and to talk to your doctor about any concerns you have before using hormonal birth control.
Blood clots form when proteins in your body activate to make a makeshift plug over an injury or hole. It’s a normal part of the healing process, but blood clots can be problematic if they form in places they shouldn’t (such as in the lungs, which is called pulmonary embolism).
According to the U.S. Food and Drug Administration, out of 10,000 women who are not pregnant and do not take birth control pills, 3 to 9 will develop a blood clot. For these clots, which are most often caused by deep vein thrombosis in the legs or arms, the symptoms can include swelling and pain, and the skin may be discolored or warm to the touch.
The hormones in some forms of birth control increase your risk for blood clots, particularly in the first 6 months of use. However, nonhormonal birth control methods such as condoms, diaphragms and cervical caps do not increase your risk.